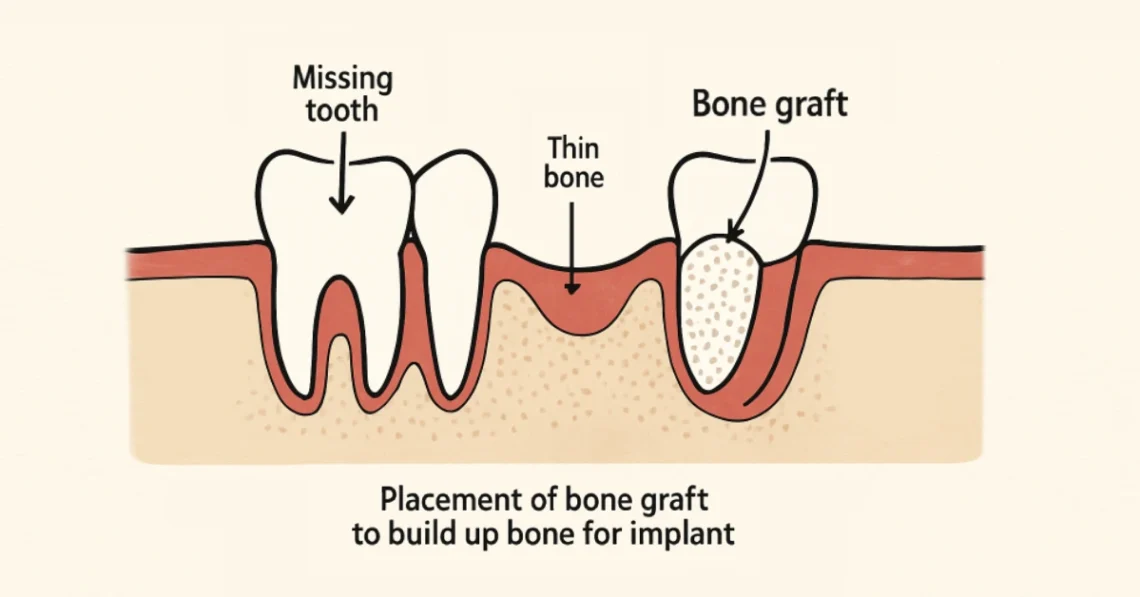
Dental implants are among the most advanced and effective solutions for replacing missing teeth, boasting both durability and a natural appearance. However, the process isn’t always straightforward—one of the most critical factors for a successful dental implant is having a strong, healthy jawbone. For patients facing bone loss due to conditions such as prolonged tooth loss, periodontal disease, or trauma, bone grafting plays a crucial role in rebuilding the jaw’s foundation.
For more information or to explore local options, visit dental implants Oklahoma City, OK. Without sufficient bone support, dental implants may not integrate properly, resulting in instability or failure. Bone grafting techniques are specifically designed to address these challenges, restoring lost bone tissue and ensuring that dental implants anchor securely, allowing patients to regain full oral function and a confident smile.
Understanding Bone Grafting
Bone grafting is a specialized surgical treatment in which new bone—either natural or synthetic—is placed into areas of the jaw lacking sufficient mass or volume. The procedure is necessary because, after a tooth is lost, the jawbone tends to resorb or shrink over time. Left untreated, this bone deterioration can make it impossible to support a dental implant safely.
For many patients, bone grafting provides the missing link between current bone levels and the threshold needed for successful dental implant integration. By essentially “rebuilding” the affected area, bone grafting creates a stable, supportive environment ready for implant placement down the line.
Types of Bone Grafts
- Autografts: Sourced from the patient’s own body, often from the hip or chin. Autografts have high compatibility and a lower risk of rejection.
- Allografts: Obtained from a human donor and rigorously processed to ensure safety. Allografts offer an effective alternative when autograft sites are not ideal.
- Xenografts: Derived from animal sources, mainly bovine. These are carefully treated for compatibility and are commonly used when human bone is limited.
- Alloplasts: Made from synthetic, biocompatible materials. Alloplasts eliminate any risk of disease transmission and can be tailored to specific needs.
Selecting the best grafting material depends on individual circumstances, patient preferences, and the clinical situation described by your dental surgeon. Each option offers unique advantages in terms of healing, safety, and availability.
When Is Bone Grafting Necessary?
Bone grafting is recommended in certain cases where the natural jawbone volume is insufficient. Common indications include:
- Loss of bone due to teeth missing for an extended period, which leads to bone resorption and thinning.
- Damage from advanced periodontal (gum) disease can progressively erode bone tissue.
- Trauma to the face or jaw, leaving defects in bone structure.
Dental professionals leverage bone grafting to regenerate lost jawbone, making dental implants viable—even for patients who previously thought implants were out of reach.
Procedure Overview
The pathway from bone grafting to a finished dental implant involves several methodical steps:
- Assessment: Dentists begin with digital imaging, such as CT scans or X-rays, to measure bone loss and plan the grafting approach.
- Graft Placement: During surgery, the graft material is positioned precisely within the deficient area. The site is then covered and allowed to heal.
- Healing Period: A healing period is required for the bone graft to integrate, a process known as “osseointegration,” where new bone cells grow into and around the graft, thereby reinforcing the jaw.
- Implant Placement: After sufficient healing, typically several months, the dental implant is placed into the newly strengthened jawbone to support an artificial tooth.
This careful, staged process significantly increases the odds of a healthy, lasting implant.
Advancements in Bone Grafting Techniques
Recent years have seen a remarkable evolution in both materials and techniques for bone grafting. For example, researchers have developed a unique glue gun that can 3D print bone-like grafts directly onto jaw fractures, potentially transforming how oral surgeons approach rebuilding bone structure. Advancements like this promise faster healing, minimal invasiveness, and higher success rates for patients needing bone augmentation.
Benefits of Bone Grafting for Dental Implants
- Enhanced Implant Stability: By restoring deficient bone, grafts provide a consistent and robust foundation, shielding implants from movement or failure.
- Improved Aesthetics: Rebuilding bone volume restores natural facial contours, preventing the aged or sunken look often associated with jawbone loss.
- Expanded Eligibility: Bone grafting enables individuals who might otherwise be turned away from implant treatment to receive the benefits of modern restorative dentistry.
Patients gain not only functional restoration but also renewed confidence in the look and strength of their smiles.
Final Thoughts
Bone grafting is a cornerstone of modern dental implantology, empowering patients with compromised jawbones to achieve reliable, natural-looking tooth replacements. As surgical techniques and materials advance, success rates continue to improve, offering more patients hope for lasting dental health and restored smiles. Consulting with an experienced dental professional is essential to determine the best approach tailored to your specific needs and goals.
Key Takeaways
- A sufficient jawbone is crucial for the successful placement of dental implants and their long-term stability.
- Bone grafting restores lost bone tissue, creating a strong foundation for implants.
- Grafts can be autografts, allografts, xenografts, or synthetic, chosen based on patient needs and clinical considerations.
- Bone grafting is often necessary after tooth loss, periodontal disease, or facial trauma.
- The process involves assessment, graft placement, healing, and eventual integration of the implant.
- Advances in grafting techniques improve healing, success rates, and patient outcomes.
- Bone grafting enhances implant stability, restores facial contours, and expands eligibility for dental implants.